Here in Hawai‘i, we’re lucky to live on beautiful islands with multigenerational families in multicultural communities. We have city life, country life, sunshine every day and some of the best food in the world. But our lifestyle, diet and even our genes can put us at risk for cancer. Yes, even here in paradise.
Cancer is a big problem. But it isn’t just one problem. It isn’t even one disease. It’s hundreds of diseases that touch millions of lives. There were an estimated 18.1 million cancer cases around the world in 2020. Of these, 9.3 million cases were in men and 8.8 million in women.
According to the American Cancer Society (ACS), one in two men and one in three women in the US will be diagnosed with cancer in their lifetime and cancer will cause the death of one in five Americans.
In Hawai‘i, it is estimated that there will be 7,730 new cases of cancer and 2,590 cancer deaths this year. Today, tomorrow and each day of the year, 20 people will be diagnosed with cancer; seven people will die from it. Sadly, these nameless, faceless statistics may hit close to home.
In this article, we’ll introduce you to people who are on a cancer journey and others who are working to help them in different ways. We’ll focus on folks here in Hawai‘i, with an emphasis on men. And we’ll highlight actions we can all take to reduce our risk for cancer and improve our lives. This article endeavors to relay accurate, helpful information with an eye toward a hopeful future. Because the future does look hopeful. At present, a lot more people are living with cancer than dying from it. There are nearly 17 million cancer survivors in the US and more than 62,000 people are living with cancer in Hawai‘i.
Over the last 30 years, cancer deaths have decreased by 29 percent due to lifesaving cancer research, increased screening, enhanced diagnostics, improved care and less tobacco use.
While cancer deaths are on the decline, cancer incidence is on the rise. As the global population grows and life expectancy increases, cancer is projected to increase to 30 million new cases worldwide in 2040. In other words, the “big problem” is projected to get even bigger.
 RESEARCH IN HAWAI‘I
RESEARCH IN HAWAI‘I
Looking for the cure for cancer can be like opening a box only to find another box. But researchers are thinking outside these boxes to unlock the mysteries of this enigmatic disease.
In Hawai‘i, more than 600 local families (2,266 people) are participating in the Hawai‘i Colorectal Cancer Family Registry Cohort, an international research project that’s studying the impact of genetics and lifestyle factors on the risk of colorectal cancer which is the third most frequently diagnosed cancer in the state of Hawai‘i.
People diagnosed with colorectal cancer, as well as family members who are affected and unaffected, will help doctors better predict the risk for colorectal cancers and find new ways to prevent them. The study revealed that some family members were at risk for colorectal cancer — but didn’t know it — and received additional testing paid for by the research study.
“Data from the registry identified new genetic mutations that had not been categorized as causing colon cancer,” says Dr. Loïc Le Marchand, PhD, the associate director for ethnic diversity at the University of Hawai‘i Cancer Center (UHCC). “These findings are significant and clinically relevant to the study of cancer risk — especially for different racial/ethnic groups.”
WHO IS AT RISK FOR DEVELOPING CANCER IN HAWAI‘I
What determines who will get cancer and who won’t? Are lifestyle, diet and race/ethnicity factors? To better understand the roles that lifestyle, diet and genetics play in cancer and other chronic diseases, researchers at the UH Cancer Center and the Keck School of Medicine of the University of Southern California began collecting data from 215,000 men and women aged 45 to 75 in Hawai’i and California in five racial/ethnic groups: Japanese American, Native Hawaiian, African American, Latino and white.
The Multiethnic Cohort (MEC) Study, which began in 1993, continues today with about half its participants still living. The large number of participants and long span of the research have generated an invaluable body of data from the most ethnically diverse study of its kind.
A key part of the study was the collection of blood and urine samples from 75,000 participants in the early 2000s. Investigators have used the samples to take measurements “that may be predictive of the occurrence of cancer — not only to better understand who will develop cancer, but to understand the mechanisms,” says Dr. Le Marchand, the principal investigator.
The MEC Study, funded by the National Cancer Institute (NCI), has brought $150 million to Hawai‘i through federal research funding. To date, more than 850 scientific articles have been published using its data to advance the understanding of cancer risk, reduce health disparities and discover new and more effective ways to prevent cancer among all people.
Multiethnic Cohort (MEC) Study Findings
■ Native Hawaiians and Japanese Americans are at higher risk of pancreatic cancer.
Among all ethnic/racial groups in Hawai‘i, Native Hawaiians and Japanese Americans have a higher risk of developing pancreatic cancer. Previous studies have shown that African Americans are at increased risk as well. But the MEC Study gives scientists data to evaluate risk, incidence and mortality rates compared to lifestyle, diet and genetics among additional ethnic/racial groups in Hawai‘i.
■ Native Hawaiians and Japanese Americans have a higher risk of liver fat.
Native Hawaiians and Japanese Americans are known to be at greater risk for liver fat and conditions associated with it. A new investigation found a genetic link between liver fat and a variant on chromosome six, which is found in Japanese Americans and Native Hawaiians, and legumes are high-quality foods that were assigned higher dietary data scores in the study. Red and processed meat, alcohol, refined grains, sodium and sugar-sweetened beverages (e.g., sodas) are foods that the study recommends we eat less of.
■ There are racial/ethnic differences in ovarian cancer risk.
A recent study using data from the MEC showed large differences in ovarian cancer risk between racial/ethnic groups. Compared to white women, the risk for Native Hawaiians was 36 percent higher. For Japanese Americans and Latinas, the risk was 21 percent and 26 percent lower. For African Americans, the risk was similar to that in whites.
■ Diet relates to the risk of colorectal cancer.
A high-quality diet was related to a reduction of colorectal cancer in men (from 16 percent to 31 percent) and women (from 4 percent to 18 percent). Fruits, vegetables, whole grains, nuts and lower level of body fatness in Japanese Americans than other ethnic groups. Visceral (VAT) and liver fat, adjusted for total adiposity, differs by race and is highest among Japanese Americans and lowest among African Americans. A better understanding of the causes of these risk factors may lead to new methods of prevention and treatment. And ongoing research to develop blood markers of visceral and liver fat may help to identify high risk individuals.
■ Processed and grilled meats are linked to an increase in cancer incidence.
People who consume the greatest amount of processed meats, such as hot dogs and sausages, had a 67 percent higher risk of developing cancer over those with the lowest consumption. A diet rich in pork and red meat may increase pancreatic cancer risk. One key takeaway is that a healthy diet includes a variety of foods in moderation.
■ Race/ethnicity is a risk factor for obesity-related cancers and metabolic diseases.
Body mass index (BMI) carries different risks for cancer across ethnic groups. Its effect on breast cancer risk is stronger and observed at a not in African Americans, European Americans or Latinos. Identifying genetic variants for liver fat will help in the development of new strategies for prevention and early detection of liver disease and related outcomes.
■ Additional findings:
Alcohol consumption, even in low amounts, increases breast cancer risk. Smoking also increases the risk of breast cancer. Lung cancer risk due to smoking is greater in Native Hawaiians and African Americans. Smokers with newly discovered genetic markers have a higher lung cancer risk.
Ka‘ana Like Mana‘o: KĀNE VS CANCER
Native Hawaiian men (kāne) have the highest death rate from colon cancer among all ethnic groups in Hawai‘i. Yet, 90 percent of colon cancer can be prevented by early and regular screening. Early screening can detect cancer at an earlier stage, lead to effective treatment and result in a better outcome. But low screening rates among Native Hawaiian men can place them at risk for late stage diagnoses and death.
“Native Hawaiian men are not diagnosed as much with colorectal cancer. But they die more often,” says Kevin Cassel, doctor of public health and principal investigator of “No Ke Ola Pono o Nā Kāne” (for the good health of men), a research study at the UHCC.
 Using culturally grounded approaches based on Native Hawaiian traditional practices of hale mua (men’s house) and community hui kūkākūkā (discussion groups), the study investigated why nearly 60 percent of Native Hawaiian men over age 50 had never been screened and 30 percent had not discussed colon health or screening with their doctors — in spite of disproportionately higher rates of cancer, diabetes, cardiovascular diseases and obesity among Native Hawaiians.
Using culturally grounded approaches based on Native Hawaiian traditional practices of hale mua (men’s house) and community hui kūkākūkā (discussion groups), the study investigated why nearly 60 percent of Native Hawaiian men over age 50 had never been screened and 30 percent had not discussed colon health or screening with their doctors — in spite of disproportionately higher rates of cancer, diabetes, cardiovascular diseases and obesity among Native Hawaiians.
The study was designed to promote healthy behaviors among 378 kāne, with an emphasis on colon cancer prevention strategies such as the fecal immunochemical test (FIT). By the end of the study, 92 percent of the kāne had improved their knowledge about colon health, 91 percent said they liked the approach and benefited from it and 76 percent agreed to complete a FIT.
“We did find a couple of men who screened positive,” says Dr. Cassel, noting that everyone who needed care received it.
Attributing to the study’s success was the fact that only men were included in the groups, and even the community volunteers who conducted peer-led conversations were Native Hawaiian kāne. Another key that led to the success of the study and its program was bringing in cultural practitioners and kūpuna (elders) who shared knowledge about traditional practices.
Another topic the men covered in the hale mua was ‘ai pono — the traditional Hawaiian diet based on fish and root vegetables, with participants discussing the relevance of those foods today. Other conversations in the hui kūkākūkā centered around pule and the importance of prayer and maintaining spiritual health.
Each community hui kūkākūkā discussion included a physician who was present to field questions. The informal setting appealed to participants who normally only see doctors during office visits.

“Once the questions started, we’d just go wherever it went,” says Nathan Wong, MD, a study kauka (physician). Dr. Wong was one of five Native Hawaiians in the first class enrolled at the John A. Burns School of Medicine on O‘ahu. Now retired from family medicine, Dr. Wong, a member of the Native Hawaiian Community Advisory Board at the UHCC, is deeply concerned about disparities that challenge Native Hawaiian men today. “There’s something going on there,” he says. “We need to see what we could do with alleviating that significant differentiation between Native Hawaiian men and others. There’s no doubt that you have significant issues with and susceptibility to many cancers.”
Expanding on issues that affect Native Hawaiian men, Dr. Wong says, “Kāne don’t go to their doctor. Perhaps they don’t trust the physician; perhaps they’re too busy. And maybe they just don’t have enough information.”
He adds that women are more accustomed to going to the doctor for themselves and their children. So this discrepancy is more than cultural or socioeconomic; it’s also gender-based. “That’s why we focused on kāne. Only guys. That’s the whole point of the hale mua.”
Dr. Wong is proud to see the community hui kūkākūkā for kāne work as “a way of bringing them together in something that’s culturally familiar — to some extent, very much Hawaiian.” And, we got more men to do their FIT tests,” he’s proud to say. Introducing FIT to kāne through community hui kūkākūkā may improve outcomes and reduce deaths. “And to me, that’s the main thing — realizing the power of groups of kāne that can discuss health in a way that is comfortable for them.”
Kākoo: KĀNE SUPPORT SERVICES
“Men are a little bit different,” says Peter Kafka, who lives on Maui and runs support groups for men. “Our minds — our emotions — work differently.” And when it comes to taking care of their own health, he says, “You know, we treat our bodies kind of like our automobile.” While describing his 1998 Toyota truck with 200,000 miles on it, Peter explains, “We’re looking to fix things. You know, when something goes awry, we get on the internet and search.” And that’s what Peter did when he was told that he had an aggressive form of prostate cancer.
Peter’s search for information and advice from people who had walked the path before him led to a support group for cancer patients. But eight years ago, the only support groups he found on Maui were filled with women with breast cancer who talked about hairstyles and recipes, he said.
Peter’s search for a support group that he could connect with led him to the Maui-based Pacific Cancer Foundation (PCF) and a national organization called AnCan (Answer Cancer) that supported him in pioneering a movement when he began hosting an online support group for men called Men’s Talk Story. The group is still active and meets online regularly for men who are dealing with every stage of every type of cancer that want to connect and talk about their diagnosis, treatments, health insurance, relationships and more.
“We also have a group specifically for men under 60,” Peter explains. “We have an emotional support group called ‘Speaking Freely’ for just guys to talk about cancer in general and how it’s impacted their life and relationships, their work — everything. This is not just a male affliction. It strikes at the heart of a relationship. So we talk very honestly and open about things. To create a trustworthy group of guys you can connect with is really life-changing.”
And now that he’s retired as the maintenance supervisor at Haleakalā National Park, Peter has more time to talk story. “A lot of guys are uncomfortable doing Zoom meetings,” he says. “So I make myself available on the phone.” If you’d like to talk story with Peter, call 808-298-1655.
Ho‘okele: NAVIGATING A CANCER JOURNEY
What happens when your life’s journey is detoured by cancer and you come to a crossroads where you must start making choices right away? You meet new doctors. You hear about surgery, chemotherapy, radiation. You spend hours sifting through information on the internet.
For many people, navigating the healthcare system can be overwhelming. And having to make choices can be beyond overwhelming.
And while you have to take this journey, you don’t have to do it alone.
Patient navigators are health professionals who focus on providing education, guidance and assistance to help patients find their way through the healthcare system and to ensure that their healthcare needs are met. The PCF offers free patient navigation services for people on Maui, Lāna‘i and Moloka‘i.
“Everybody’s cancer journey is different,” says PCF Executive Director Nancy La Joy, who describes a patient navigator as “a lot like a social worker and a community health worker who really walks the journey with each person, one by one, hand in hand.”
Personalized care can make all the difference for a patient’s outcome.
“The patient navigator’s job is to eliminate any barriers to healthcare,” says Nancy, “Those could be educational, advocacy, understanding your diagnosis, understanding your treatment plan, understanding your medical team, and what the role is of each of the players.”
Transportation is one of the biggest barriers to healthcare, says Nancy. “A lot of times, during the course of treatment, people will get to the point where they don’t feel well enough to drive themselves. Or maybe they need to go to O‘ahu or the mainland for specialized treatment. We help with all of that — ground transportation, air transportation, and sometimes lodging.” When travel is necessary, the PCF will work with patients, insurance companies and service providers, including airlines and hotels, to find solutions.
PCF’s goal is, “to help people get through treatment without any trouble or missed appointments, missed opportunities for care — feeling better and doing better and getting on with your life,” says Nancy, noting that navigators also help people learn to live with cancer for months and years. Throughout the pandemic, the PCF has continued to provide free services through support groups, meditation classes, nutritional support, and its largest program — patient navigation.
Hale o Ka Mana‘olana: BUILDING HOPE
 The American Cancer Society is built on hope. Its mission is to save lives, celebrate lives and lead the fight for a world without cancer. And one way the organization does that is by providing a free place for patients and caregivers to stay when they need to travel for cancer treatment — because often, the best hope for effective treatment is far from home.
The American Cancer Society is built on hope. Its mission is to save lives, celebrate lives and lead the fight for a world without cancer. And one way the organization does that is by providing a free place for patients and caregivers to stay when they need to travel for cancer treatment — because often, the best hope for effective treatment is far from home.
There are more than 30 places in the US known as Hope Lodge.
The Clarence T.C. Ching Hope Lodge Hawai‘i in Honolulu opened in 2016 as the first and only Hope Lodge in the western US.
For nearly 1,000 cancer patients and their caregivers who’ve traveled from Hawai‘i Island, Maui, Lana‘i, Moloka‘i, Kaua‘i, Guam, American Samoa, and other Pacific Islands for cancer care on O‘ahu, Hope Lodge Hawai‘i has been a safe, caring, comfortable home away from home.
An average stay at Hope Lodge Hawai‘i is 14 nights. And by offering more than 5,000 nights of accommodations each year — free-of-charge — the ACS provides an annual benefit to cancer patients in Hawai‘i and the Pacific totaling more than $1.2 million. That’s a big help and a big comfort in a place built on hope.
Nā Mea No‘ono‘o Hana: LATEST INNOVATIONS FOR LIFE
Through innovations in cancer care in Hawai‘i, doctors have access to better tools that are giving patients better outcomes.
PET/CT (positron emission tomography/computed tomography) scans are key in detecting, staging and monitoring for recurrence of cancer.
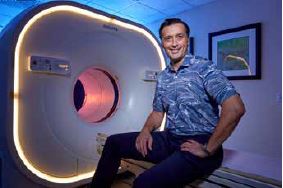 Advanced medical imaging technology is now available in Hawai‘i, offering increased speed and quality for doctors, and enhanced comfort and safety for patients.
Advanced medical imaging technology is now available in Hawai‘i, offering increased speed and quality for doctors, and enhanced comfort and safety for patients.
“Accurate diagnostic data can provide a roadmap for the treating physician to best assess a treatment protocol,” says Insight Imaging President Massimiliano “Max” Clini.
“Better scans lead to better data which lead to better care.”
The latest innovations in digital PET/CT scanners reduce the amount of radiation exposure to patients by up to 50 percent while reducing scan times by up to 90 percent. “Older technology would require patients to lie down on the scanner for upwards of 45 minutes,” explains Max. And that was the case just a few years ago. Today, cutting-edge diagnostic scans can be completed in less than 10 minutes.
State-of-the-art digital imaging can also benefit patient care. “The opportunity to detect smaller lesions can lead to earlier detection of cancers,” says Max, showing how innovative advancements in diagnostic tools can improve the success rate of
cancer treatments.
E Ho‘oikaika Imua: STRIVING FOR A BRIGHT FUTURE
The UH Cancer Center just celebrated 50 years of progress through cancer research, education and community outreach, as well as 25 years of continuous designation by the NCI.
“This is Hawai‘i’s cancer center,” says UHCC Interim Director Joe W. Ramos, PhD. “We focus on: How can we help Hawai‘i? How do we reduce the burden of cancer here? How can we better identify their causes here and use that knowledge to prevent cancers?” And just as urgently, Dr. Ramos adds, “How can we use that knowledge to attack cancers with these new therapeutics and new diagnostics?”
“We’re trying to figure out what makes different cancers form, grow, and move and metastasize,” explains Dr. Ramos. “If you can catch the cancer early, you have more options for successful treatment and a cure — if it’s early enough. But the problem is, if you catch it later, it may have already spread to other locations. So we’re working hard to better prevent, diagnose and treat cancer.”
To address these issues,” Dr. Ramos says, “We have great faculty and staff working specifically for Hawai‘i and the USAPI.” He describes the UHCC faculty as among the top in the country. And they’re bolstered by strong partnerships with local hospitals and healthcare groups, support from the state legislature and funding through grants that acknowledge the center’s high-quality faculty and top-level ranking as a world-class research institute.
What will success look like for the UHCC in the future? It will be as diverse as the populations it serves, with cutting-edge technologies, innovative research, expanded access to clinical trials here in Hawai‘i, an Early Phase Clinical Research Center, and a high-tech Organoid Generation Facility that will help ensure that Hawai’i continues to have one of the leading cancer research institutions in the nation and the world for the next 50 years.
Filled with hope, ACS Hawai‘i Board Chair Shane Morita, MD, also sees the promise of new technologies and innovations.
“I think the future is really bright,” he says. “We’re looking at different ways of treating cancer with immunotherapy and targeted therapy. There are breakthroughs being made every day.”
As medical director for surgical oncology at The Queen’s Medical Center, Dr. Morita draws inspiration from personal experience — his father died of cancer and his mother became a caregiver. And through professional experience, he sees a
path to a cure through clinical trials.
“They pave the way to find the next standard of care — the gold standard of how we treat patients,” adds Dr. Morita. “When I was training at the National Institutes of Health, a lot of the clinical trials that I was involved in were proven to be effective and have become the standard of care.”
Komo i Ka Noi‘i: JOIN A STUDY OR CLINICAL TRIAL
Would you like to help to advance scientific knowledge and have an impact on the fight against cancer? If you participate in a research study or clinical trial at the UHCC, you might play a role in the discovery of new ways to detect, diagnose, and treat cancer and other diseases, and reduce the chance of developing them in the first place. Volunteers of all ages and ethnicities are needed, and recruitment opens up for different projects at different times. To learn more, call the UHCC at 808-586-2979.
 Clinical Trials Actively Recruiting Participants
Clinical Trials Actively Recruiting Participants
■ Cyanotoxin Trial
There’s an urgent need to investigate cyanobacteria (blue-green algae) because men and women in Hawai‘i and Guam have some of the highest rates of liver cancer in the US; Native Hawaiian men and CHamoru men have the highest risk of liver cancer. The UHCC is recruiting 400 adults — especially Native Hawaiian men — aged 40 to 70 with no prior cancer.
■ Mediterranean Diet Trial
Researchers at the UHCC are looking for 240 Asian, Native Hawaiian/Pacific Islander and white people in Hawai‘i to go on a Mediterranean diet (seafood, vegetables, fruits, whole grains, beans, nuts and olive oil) or an intermittent energy restriction diet for six months for weight loss.
■ Breast Screening Study
Women 45 to 74 who are planning to get a mammogram are invited to join a research study and help improve future breast screening. The TMIST Breast Screening Study will compare 2-D and 3-D mammography and build a tissue bank for research that can help personalize screening based on personal risk factors and genetics.
■ Caregiver Study
Eligible caregivers, family members or friends of newly-diagnosed colorectal cancer patients may be eligible to receive a tablet with educational materials. Participants may keep the tablet when the study concludes. Researchers want to learn whether providing an educational curriculum in this way can improve quality of life for patients and their caregivers.
Noho Ana Maika‘i a Hau‘oli: LIVING WELL WITH CANCER
Brad Lum says he’s glad that he learned he had Stage 4 prostate and bone cancer eight years ago. If he hadn’t been told that then, he wouldn’t be living his best life now.
“Cancer isn’t the most important thing in my life,” insists Brad. “It is there. I acknowledge it. That’s about it.”
 Active and fit, Brad enjoys hiking, surfing and going to the gym. He’s becoming vegan. And he encourages people to eat foods like kalo, ‘ulu, and ‘ōlena (turmeric) that were cultivated in Hawai‘i. Brad also strives to balance Western medicine with traditional Hawaiian la‘au lapa‘au. “You can do both,” he says. “Make it balanced.”
Active and fit, Brad enjoys hiking, surfing and going to the gym. He’s becoming vegan. And he encourages people to eat foods like kalo, ‘ulu, and ‘ōlena (turmeric) that were cultivated in Hawai‘i. Brad also strives to balance Western medicine with traditional Hawaiian la‘au lapa‘au. “You can do both,” he says. “Make it balanced.”
Kumu Brad keeps his balance through chant and prayer. Around the time of his cancer diagnosis, he realized, “I started to see clearly.” And that’s when he became a Buddhist.
The kumu hula and retired teacher is also glad to be making plans for his 70th birthday. “I’m gonna have two parties,” he says. “And I’m gonna jump out of a plane.”
For all his positivity, Kumu Brad keeps it real and he keeps it balanced. “I just wanna enjoy life,” he says. “Just enjoy, period.”
Cancer is a big problem. And our lifestyle, our diet, and even our genes can put us at risk to be among the one in two men or one in three women who will be diagnosed with cancer in our lifetime.
So take actions that will reduce your risk. Go for a walk. Smell the flowers. Keep informed. Eat more vegetables. Lose weight. Use sunscreen. Stop smoking. Join a research study. Enjoy the views. Keep in touch with friends and family. Stay balanced. And just enjoy life, period.
UNIVERSITY OF HAWAI‘I CANCER CENTER (UHCC)
701 Ilalo St., Honolulu, HI 96813
808-586-3010 | info@cc.hawaii.edu
www.uhcancercenter.org
UH CANCER CENTER CLINICAL TRIALS OFFICE
808-586-2979 | CTOAdmin@cc.hawaiil.edu
AMERICAN CANCER SOCIETY – HAWAII
Cancer Helpline: 800-227-2345
https://www.cancer.org/about-us/local/hawaii.html
CLARENCE T.C. CHING HOPE LODGE HAWAI‘I
251 South Vineyard Street , Honolulu, HI 96813
808-566-8430
PACIFIC CANCER FOUNDATION
95 Mahalani St., Ste. 8, Wailuku, HI 96793
808-242-7661 | admin@pacificcancerfoundation.org
www.pacificcancerfoundation.org
MEN’S TALK STORY SUPPORT GROUP
Peter Kafka, 808-298-1655
www.ancan.org/maui-mens-group
www.pacificcancerfoundation.org/mens-talk-story
ANCAN
(The home of peer-to-peer virtual support groups)
415-505-0924 | info@ancan.org
www.ancan.org


Leave a Reply