Making healthy dietary choices can help you feel your best and stay active. It can also help you lower your risk of developing some health conditions that are common among older adults.
The US Food and Drug Administration (FDA) has a tool to help you make informed food choices that can have positive effects on your health and wellness. It is called the Nutrition Facts label and you can find it on packaged foods and beverages.
 Understanding the Nutrition Facts Label
Understanding the Nutrition Facts Label
The following key terms are intended to make it easier for you to use the Nutrition Facts labels to make informed food choices.
[1] Servings Per Container shows the total number of servings in the entire food package or container. One package of food may contain more than one serving. For example, if you eat or drink two servings, you are getting double the calories and double the nutrients that are listed on the label.
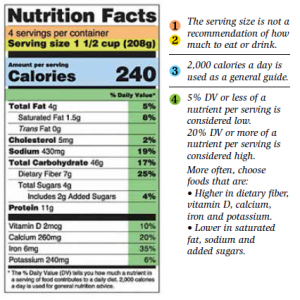
[2] Serving Size is based on the amount of food that is usually eaten at one time. Serving size is not a recommendation of how much to eat. The nutrition information listed on the label is usually based on one serving of the food; however, some containers may also have nutrition information listed for the entire package.
[3] Calories refers to the total number of calories in a serving of the food. To achieve or maintain a healthy body weight, balance the number of calories you eat and drink with the number of calories your body burns.
The general guide for calorie consumption per day is 2,000. Your calorie needs may be higher or lower and vary depending on your age, sex, height, weight and physical activity level. Check your calorie needs at www.ChooseMyPlate.gov/MyPlatePlan.
[4] %Daily Value (%DV) shows how much a nutrient in a serving of the food contributes to a total daily diet. The Daily Values are reference amounts (in grams, milligrams or micrograms) of nutrients to consume or not to exceed each day.
Use the %DV to determine if a serving of the food is high or low in an individual nutrient. You can also use the %DV to compare food products (make sure the serving size is the same). For example, if you eat one serving of a food and it provides 10% DV of dietary fiber, then for that day, you have eaten 10% of your dietary fiber daily goal.
 As a general guide, 5% DV or less is considered low; 20% DV or more is considered high.
As a general guide, 5% DV or less is considered low; 20% DV or more is considered high.
Nutrients and Your Needs
Nutrients are substances in your food that keep your body working well. Eating too much or too little of some nutrients may increase your risk of certain chronic conditions, such as heart disease and high blood pressure.
Older adults have different nutritional needs than other age groups. The Nutrition Facts label can help you monitor some of the nutrients in your diet.
 Get More of These Nutrients: Dietary Fiber, Vitamin D, Calcium and Potassium
Get More of These Nutrients: Dietary Fiber, Vitamin D, Calcium and Potassium
Many older adults do not get the recommended amount of these nutrients. Compare and choose more foods in order to get more of these nutrients on most days.
Dietary fiber is a type of carbohydrate that cannot be easily digested. It can speed up the movement of food and waste through the body, increasing the frequency of bowel movements. Diets higher in dietary fiber may reduce the risk of developing cardiovascular disease. The Daily Value for dietary fiber is 28 grams (g) per day.*
Calcium is a mineral that is important for bone health. It also helps with muscle and nerve function, blood clotting and hormone secretion. Diets higher in calcium can reduce the risk of developing osteoporosis (weak and brittle bones). The Daily Value for calcium is 1,300 milligrams (mg) per day.*
Vitamin D helps your body absorb calcium and is important for bone health. It also plays a role in blood pressure management, hormone production, and immune and nervous system function. Diets higher in vitamin D can reduce the risk of developing osteoporosis (weak and brittle bones). The Daily Value for vitamin D is 20 micrograms (mcg) per day.*
Potassium is a mineral that helps with fluid balance and heart, muscle and nervous system function. The Daily Value for potassium is 4,700 mg per day.*
 Consume Less of These Nutrients: Saturated Fat, Sodium and Added Sugars
Consume Less of These Nutrients: Saturated Fat, Sodium and Added Sugars
Most older adults get too much of these nutrients. Compare and choose foods in order to consume less of these nutrients each day.
Saturated fat is found in higher amounts in animal products. An exception is seafood, which is generally low in saturated fat. Unsaturated fats are found in higher amounts in plant-based oils (e.g., canola and olive oils), nuts, seeds and seafood. Diets in which unsaturated fats are eaten in place of saturated fats and within the recommended daily limits for calories are associated with a reduced risk of developing cardiovascular disease. The Daily Value for saturated fat is less than 20 g per day.*
Sodium is a mineral commonly found in table salt and in many commercially processed, packaged and prepared foods. The body needs sodium in relatively small amounts. Sodium is important for fluid balance as well as muscle and nervous system function. Diets higher in sodium are associated with an increased risk of developing high blood pressure, which can raise the risk of heart attacks, heart failure, stroke, kidney disease and blindness. Since blood pressure often rises with age, limiting your sodium intake becomes even more important each year. The Daily Value for sodium is less than 2,300 mg per day.*
Added sugars include sugars that are added during the processing of foods (such as sucrose or dextrose), foods packaged as sweeteners (such as table sugar), sugars from syrups and honey, and sugars from concentrated fruit or vegetable juices. Diets high in calories from added sugars can make it harder to meet nutrient needs while staying within calorie limits. The Daily Value for added sugars is less than 50 g per day.*
Older adults should more often look for foods with a higher %DV of dietary fiber, vitamin D, calcium and potassium. Older adults should also look for foods with a lower %DV of saturated fat, sodium and added sugars more often. Talk to your healthcare provider about which nutrients you should track closely for your overall health.
*Based on a 2,000-calorie daily diet.
US FOOD AND DRUG ADMINISTRATION
www.fda.gov/nutritioneducation
1-800-SAFEFOOD (toll free):
MTWF, 10a–4p, Th 12:30p–1:30p EST (- 6 hrs PST)
Closed on federal holidays
Visit www.ChooseMyPlate.gov for more information about making healthy food choices.
 How It Works: The sponsor checks in with the kūpuna once a week via phone and asks if they need any food, supplies or medication (no narcotics). The sponsor will then shop and deliver the items to the kūpuna The sponsor will provide a receipt to the kūpuna for the items purchased, and the kūpuna will reimburse the sponsor for the cost of the items via cash or check (no credit cards allowed).
How It Works: The sponsor checks in with the kūpuna once a week via phone and asks if they need any food, supplies or medication (no narcotics). The sponsor will then shop and deliver the items to the kūpuna The sponsor will provide a receipt to the kūpuna for the items purchased, and the kūpuna will reimburse the sponsor for the cost of the items via cash or check (no credit cards allowed). Safety Procedures: Our Kūpuna takes the health of its clients and volunteer sponsors very seriously. The program strives to have little to no physical interaction between volunteer and kūpuna. Volunteers are required to follow a set of safety procedures recommended by Dr. Rupal Gohil in Kailua. If physical interaction is required, it is highly recommended that both parties maintain at least six feet of separation from each other. Safety procedures include but are not limited to: Pickup and delivery should be done solo. Sponsors are also not allowed to delegate this responsibility to another person. Volunteers must wash their hands or use alcohol-based hand sanitizer (at least 60 percent alcohol) before and after making a delivery. Face masks and gloves (provided) are required. Volunteers will transfer items to bags and/or boxes outside of the kupuna’s door. A reimbursement plan must be arranged prior to delivery. Kūpuna should call their pharmacy to put their credit card in their system. Kūpuna must disinfect items upon receiving them.
Safety Procedures: Our Kūpuna takes the health of its clients and volunteer sponsors very seriously. The program strives to have little to no physical interaction between volunteer and kūpuna. Volunteers are required to follow a set of safety procedures recommended by Dr. Rupal Gohil in Kailua. If physical interaction is required, it is highly recommended that both parties maintain at least six feet of separation from each other. Safety procedures include but are not limited to: Pickup and delivery should be done solo. Sponsors are also not allowed to delegate this responsibility to another person. Volunteers must wash their hands or use alcohol-based hand sanitizer (at least 60 percent alcohol) before and after making a delivery. Face masks and gloves (provided) are required. Volunteers will transfer items to bags and/or boxes outside of the kupuna’s door. A reimbursement plan must be arranged prior to delivery. Kūpuna should call their pharmacy to put their credit card in their system. Kūpuna must disinfect items upon receiving them.


















