Despite hospice care’s increasing popularity, there are still widely held misconceptions regarding end-of-life care. This article by members of the Society of Certified Senior Advisors (www.csa.us) seeks to dispel many myths about hospice care and to present accurate information on this growing segment of our healthcare system. By doing so, it is hoped that hospice benefits will be accessed more widely.
Despite hospice care’s increasing popularity, there are still widely held misconceptions regarding end-of-life care. This article by members of the Society of Certified Senior Advisors (www.csa.us) seeks to dispel many myths about hospice care and to present accurate information on this growing segment of our healthcare system. By doing so, it is hoped that hospice benefits will be accessed more widely.
MYTH: Hospice care is appropriate only in the last few days of the life of a terminally ill.
A common misconception is that hospice care is a comfort measure only in the last few days of life of a terminally ill patient. The hospice benefit is actually for patients who have a terminal illness with a life expectancy of six months or less. Hospice care helps people with life-limiting illnesses to live their final months in comfort and with dignity. Two physicians — the attending physician and the hospice physician — must certify the primary terminal illness, as well as agree that following the natural course of the illness, the patient’s life expectancy is six months or less. Patients are eligible for hospice care after this physician certification. If at this time, a person is not yet ready to proceed with hospice care, a hospice referral can be placed at a later time. Given that no one can accurately predict the time of death for a terminally ill patient, the hospice benefit allows patients to remain in the program as long as they continue to meet the criteria.
When deciding on whether or not to proceed with hospice care, it is important for the patient and family to have a conversation with their medical team regarding goals of their care. Also, patients and families need to know what medical care is available to them, as well as the risks and benefits associated with that care. For example, if there is a curative treatment option the patient is interested in trying, then the goal of care would not be in line with the hospice/palliative care approach. Discussion related to goals of care can assist patients and their families in naming what is important to them, both medically and in relation to their quality of life at that time.
 MYTH: Mostly cancer patients go into hospice.
MYTH: Mostly cancer patients go into hospice.
The Centers for Medicare and Medicaid Services has reported relatively fewer cancer patients and relatively more non-cancer patients as a percentage of total hospice patients. In 2006, non-Alzheimer’s dementia became the most common diagnosis among Medicare hospice patients. Alzheimer’s disease accounts for 70 percent of dementia cases. Over half of all those who live past 85 develop some form of dementia. Over five million Americans are currently living with Alzheimer’s disease, and by 2050, that number will rise to 13.5 million. At the final phase of the dementia patient’s life, hospice care provides timely and compassionate support for the patient and family.
MYTH: Hospice care shortens lifespan.
How could we experience dying — our own and that of our loved ones — with less anxiety and and with greater openness, and peace of mind? Research suggests that hospice holds a key. There is evidence that care aimed at comfort and quality of life actually extends life rather than shortens it, and enables a more comfortable death, as well.
MYTH: Having early family conversations about end-of-life care is “giving up” on living.
Often, patients and families feel like they are giving up when deciding to enroll into hospice care. It’s true that the highest percentage of hospice patients, 27.9 percent, are on hospice care for only seven days or less. But hospice admission criteria reveal that the benefit is intended to provide care for much longer than a few days — up to six months. Patients and family members indicate that they would like to receive information about hospice care soon after the terminal diagnosis. Learning about the hospice philosophy and the services provided can be beneficial for patients and families while they decide how to proceed with their medical care after a terminal diagnosis. With an early hospice consultation, along with early discussion on end-of-life care, families can take advantage of benefits of hospice care more fully, enjoying a much better quality of time together during the patient’s remaining time.
MYTH: Pain medication will make patients overly sedated and addicted to opioids.
Up to 80 percent of people will experience some sort of pain during the dying process. But patients seem apprehensive about pain management and medication use at the end of life.
Patients and their families often fear addiction and side effects such as over-sedation. However, if a patient is in severe pain, opioid-based pain medications are the gold standard treatment.
Opioids relieve both pain and shortness of breath. The morphine dose can be slowly increased for comfort, and often, patients are able to self-administer the drug in amounts that fit their individual pain or breathing needs.
Patients and their families may also delay the use of opioids out of fear that use of pain medication indicates that death is imminent. This is not true. Opioids can be increased, as tolerated, to manage pain. Dose adjustment, and appropriate monitoring and management of adverse reactions continue for all patients who use any sort of opioid in order to ensure patient safety.
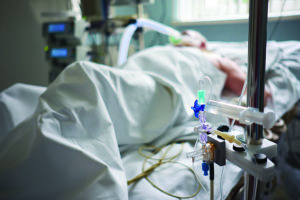 MYTH: Hospice must provide the patient food and fluids until the moment of death.
MYTH: Hospice must provide the patient food and fluids until the moment of death.
At the end of life, hunger tends to be absent. When people can no longer eat or drink independently, body systems are shutting down; they have become unable to use the calories in food. Family understandably may be concerned that if the patient is not being fed, he or she is being starved to death. But when people become too weak to swallow, they will cough or choke on what they try to eat or drink. This can lead to fluids and food entering the lungs, and possible infection. Providing food and fluids at this point usually requires a feeding tube placed surgically through a hole in the abdomen to the stomach. So it is critical for patients to appoint a healthcare decision-maker and discuss their preferences regarding artificial nutrition and hydration.
MYTH: Hospice care is an expensive burden.
Misunderstood aspects of hospice care include payment and the services covered under the hospice care benefit.
Medicare is the primary source of payment for the hospice benefit. If a patient is on a Medicare Advantage plan, it reverts to original Medicare for payment of hospice care. In order to utilize payment by Medicare for the hospice benefit, patients must be eligible for Medicare Part A, choose a Medicare-certified hospice agency, and have a terminal illness with a life expectancy of six months or less as certified by two physicians. The Medicare benefit then covers hospice services at a 100 percent per diem rate. Hospice can take place in a private home, nursing home, assisted living or residential hospice home. Medicare is not the only payment source for the hospice benefit. Many private insurance companies cover it, as well.
Important Conversations
As a patient approaches death, treatments intended to cure a disease may no longer serve his or her goals or best interest. The decision to stop, withhold or forgo curative treatments to focus on comfort measures and quality of life is difficult for all involved. So it is vital to have detailed conversations with your healthcare decision-maker before these choices become imminent.
The hospice benefit allows patients to die peacefully, but more importantly, to live their life according to their own goals. Education and discussions among family members can provide clarity regarding end-of-life and hospice care, preparing loved ones to make informed decisions.
Will your loved ones know what you value at the end of your life? Talk to them today.
This edited article is shared courtesy of the
SOCIETY OF CERTIFIED SENIOR ADVISORS®
800-653-1785 | Society@csa.us
www.csa.us
 If you’re a small business owner or you work for one, the Social Security Administration’s (SSA) online suite of services can help make life easier. Our business services allow you to file W-2/W-2Cs online and verify your employees’ names and SS numbers against our records.
If you’re a small business owner or you work for one, the Social Security Administration’s (SSA) online suite of services can help make life easier. Our business services allow you to file W-2/W-2Cs online and verify your employees’ names and SS numbers against our records.