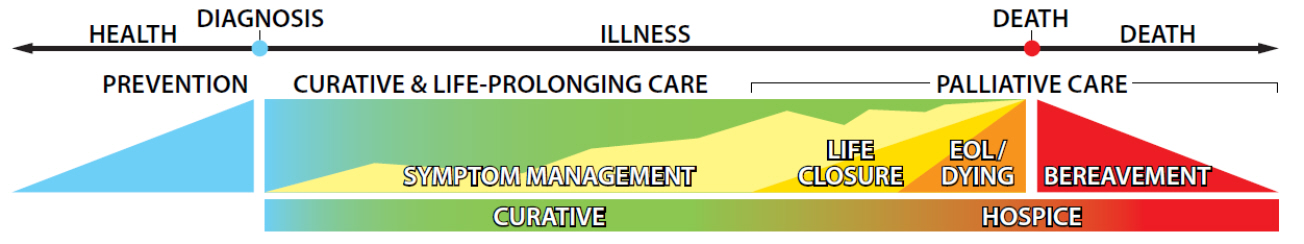
Dame Cicely Saunders (founder of the first modern hospice in London in 1968) summed up the hospice philosophy best when she told her patients:“You matter to the last moment of your life, and we will do all we can, not only to help you die peacefully, but to live until you die.” Hospice care is a model for quality compassionate care for people facing a life-
Who is eligible for hospice care?
When the goal of treatment begins to shift from cure to providing comfort, it may be time to consider hospice for persons facing terminal cancer: end-
Where is hospice care provided?
Most hospice care is provided in a person’s own home. Hospitals, nursing homes, assisted living, care or foster homes are other possible settings.
What services are covered under hospice care?
- Nursing: pain and symptom management
- Personal care/home health aide
- Social services
- Spiritual counseling
- Volunteers
- Respite care
- Bereavement support
Who pays for hospice?
Medicare, Medicaid and all medical insurances offer hospice benefit. Durable medical equipment and medications related to the terminal diagnosis are covered. Little or no co-
What is palliative care?
According to the World Health Organization (WHO), palliative care is an approach that improves the quality of life of patients and their families facing the problem associated with life-
How is hospice different from palliative care?
Palliative care is specialized care for persons with life-
What is supportive or concurrent care?
“Supportive” or “concurrent” care is a type of palliative care that encompasses all the extra care provided in addition to regular medical care by a full team of physicians, nurses, social workers, chaplains, and aides who specialize in caring for people facing serious illness. This means that somebody with a serious illness can have all the benefits of comfort care and still receive life prolonging treatments.
Who pays for Supportive or Concurrent Care?
Hawaii Medical Service Association (HSMA) offers supportive care services for homebound members who have advanced cancer, advanced heart failure or emphysema. University Health Alliance (UHA) offers concurrent care services to persons with any serious illness. HSMA and UHA have partnered with local hospices to offer this innovative program.


 Osteoarthritis (OA) is one of the most common forms of arthritis. About 27 million people in America have osteoarthritis. It is a chronic condition in which the material that cushions the joints, called cartilage, breaks down. This causes the bones to rub against each other, causing stiffness, pain and loss of joint movement.
Osteoarthritis (OA) is one of the most common forms of arthritis. About 27 million people in America have osteoarthritis. It is a chronic condition in which the material that cushions the joints, called cartilage, breaks down. This causes the bones to rub against each other, causing stiffness, pain and loss of joint movement.
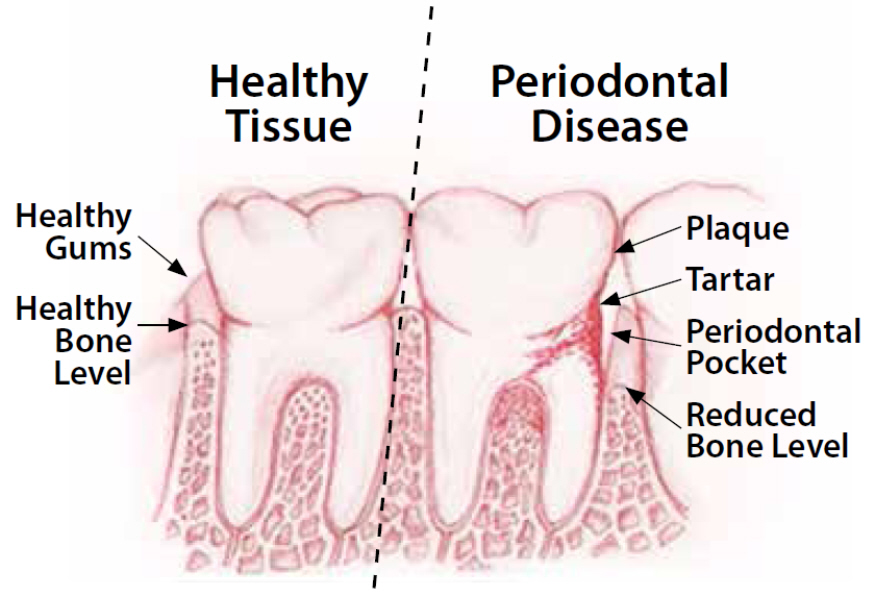 What causes periodontitis?
What causes periodontitis?